|
This section contains snippets of information about sarcoidosis and links to sites where you may read more detailed accounts
of the disease. The information I have provided here was selected from topics in which I was interested when first diagnosed and
topics of searches done by visitors to my site since I started it. Each snippet is a stand-alone piece, so there may be some
repetition of information found in other snippets. If anyone has a subject he/she would like to have me add to this
section, please feel free to contact me.
|

|
Sarcoidosis is a chronic, systemic disease. A chronic disease is one that persists for a long time,
i.e. three months or more. Chronic diseases generally cannot be prevented by vaccines or cured by medication, nor do they just disappear.
Systemic diseases are diseases that can affect number of organs and tissues, or affect the body as a whole. Of those who contract
sarcoidosis, the vast majority first notice symptoms that involve their lungs, but any or all organs in the body can be involved over
time, especially if the disease becomes chronic.
A large majority of people who are diagnosed with sarcoid, approximately 80%, will
never experience further episodes or exacerbations after the initial disease period for which they are diagnosed. Within a year
or two they will be completely free of symptoms. They will, however, never be completely cured. The disease has no known cure
and will remain in the individuals' bodies for the rest of their lives. The remainder of those who contract sarcoidosis will
continue to have symptoms and/or flare-ups of disease activity in varying levels of severity and longevity.
Severity can range from having no visible symptoms but showing positive medical test results to extremely severe symptoms that
destroy a person's quality of life.
Longevity can range from a few weeks to lifelong symptoms at erratic intervals or a progressive disease track in which a small
proportion of those
diagnosed with sarcoidosis will grow progressively sicker and require considerable medical intervention to maintain their
quality of life at a reasonable level.
Despite all medical assistance, about 5% of those diagnosed with sarcoidosis will
succumb to its debilitating effects and die. Most of those individuals have experienced complications from pulmonary sarcoidosis (lungs),
neurological sarcoidosis (central and peripheral nervous system), and cardiac sarcoidosis (heart). In particular, a person with
cardiac sarcoid may have a life-ending episode without even knowing they have sarcoidosis. It is only diagnosed when an autopsy
is performed.
|
|
Many physicians believe that sarcoidosis is a benign condition, but there were probably equally as many doctors just a decade
ago who believed that sarcoidosis is a rare disease. In today�s medical world you will not see �rare� and �sarcoidosis� used in
the same sentence very often, if ever. And in the same vein more and more medical doctors are questioning just how �benign� the
disease really is.
Information provided by the Illinois Department of Public Health
reports that "although sarcoidosis was once considered a rare disease, it [sarcoidosis] is now known to be a chronic,
common illness that appears all over the world. In fact, it is the most common of the fibriotic lung disorders."
There are two possible reasons for the previous belief that sarcoidosis was rare. First, many patients have no visible
symptoms and appear to be healthy. They are diagnosed "by accident" while being assessed for some other medical problem
or when having a routine physical exam. Various medical tests produce �positive� results. Secondly, some patients are
misdiagnosed as having any of a number of diseases that have symptoms similar to those in sarcoidosis. And additionally,
until recently the medical community and general public barely knew that there was such a disease. They needed to be
provided with accurate information so diagnoses and treatments could become more reliable. Additionally, knowledge about
sarcoid will in the future encourage provision of greater funding for research into its origins, treatment, and possible cures.
As doctors learned more about sarcoidosis, they found that it [sarcoidosis] may not be as benign as they originally thought.
These doctors felt that they needed to remain vigilant in diagnosing and managing sarcoidosis because it could be an insidious
condition that could manifest in various ways. They now know that a small number of patients will have a very gradual and
deceitfully subtle progression of the disease that never really goes into remission and eventually results in permanent damage
to one or more areas of the body. Other patients will have a relatively inactive level of sarcoidosis, but will continue to
exhibit some seemingly minor ongoing symptoms during that period. And others, who appear to be a relatively small number at
present, may have an initial episode that completely remits within a year or two, so they think they are �cured.� However,
somewhere in the future the disease returns, sometimes after ten years or more of inactivity.
The doctors in the Internal Medicine Service, University Hospital of Bellvitge, University of Barcelona, Barcelona, Spain,
conducted a study of the records of a group of 17 patients who
experienced a recurrence of sarcoidosis following complete remission and prolonged period of inactivity. The study covered 28
years and concluded that �acute sarcoidosis, and particularly L�fgren's syndrome, may recur many years after complete
remission. Consequently, a long-term follow-up is recommended even in patients with inactive disease. This clinical
observation strongly suggests that a re-exposure to or re-infection by an extrinsic antigen triggers the new flare-ups of the
disease.� Therefore, once a patient is diagnosed with sarcoidosis, he/she should be evaluated by a doctor regularly whether
symptoms are present or not. Appropriate tests for the most reliable indicators of sarcoid activity, including a complete
eye exam, should be included in such evaluations. If stability of the condition and signs of inactivity have been maintained
for longer than one year after the cessation of treatment, the possibility of relapse is considerably diminished, but the
patient and his physician should continue to be vigilant, since relapses can occur even after ten years of inactivity.
The good news is that it has been determined that such vigilance generally results in a good outcome.
|

|
Sarcoidosis is an autoimmune disease, but its actual origin is unknown. It is believed that autoimmune diseases may involve a
combination of a dominant genetic trait that occurs in about 20% of the population and an agent in the environment such as an allergen
or virus that triggers the process. With similar wording the AARDA Website states
that bacteria, viruses, toxins, and some drugs may play a role in triggering an autoimmune process in someone who already has a genetic
(inherited) predisposition to develop such a disorder. The
Foundation for Sarcoidosis Research (FSR) believes that "some research suggests that bacteria, viruses or chemicals might
trigger the disease. Although such triggers might not affect most people, it is possible that in someone with the right genetic
predisposition they provoke the immune system to develop the inflammation associated with sarcoidosis" [or some other autoimmune
disease.] According to the American Autoimmune Related Diseases Association (AARDA)
autoimmune diseases may occur in families, but may present as any one of
about a hundred different autoimmune diseases (in my case, about the time my initial symptoms appeared, my daughter was
diagnosed with mulitple sclerosis when she was in her early twenties; then I was diagnosed with fibromyalgia as a secondary
condition to my sarcoidosis; and more recently at least two of my daughter's three children have been diagnosed with celiac
disease as juveniles;). Therefore, it is important for families with members who have autoimmune diseases to mention this
fact when another member of the family is experiencing medical problems that appear to be difficult to diagnose.
|
|
A number of general symptoms may appear in those who have sarcoidosis. These include fatigue that may be extreme at
times and require the patient to get additional amounts of sleep, including naps during the day. There may be varying degrees of
depression that sometimes have a sudden onset/retreat. Muscle weakness/lethargy may be present as well as general
joint pain, most often in the knees. Low-grade fever, heat sensitivity, weight loss, and headaches are additional symptoms
that may occur in sarcoidosis. In a review of a study of sarcoid patients, Ruth Wirnsberger, University of Maastricht in the Netherlands, wrote in
"Quality of Life and Health Status in Sarcoidosis" (all 217 pgs seen at this
link) that along
with the chest-related symptoms, "patients may also suffer from nonspecific symptoms such as fatigue, fever, weight loss, and muscle pain."
"Persistent fatigue may not be taken seriously or may be underestimated by the patient's physician, family, and/or workplace." "Moreover,
about one third of the patients suffered from tension, strain, and/or depressive symptoms, which by the patients themselves were
attributed to the ongoing disorder." Ms. Wirnsberger stated that patients with sarcoid were found to be impaired with respect to
their mobility, sleep, ability to work, recreation/exercise, and social interaction. Where fatigue was a factor, metabolic derangements
and decreased respiratory muscle strength were found.
|

|
Site specific symptoms depend upon the body system or organ involved. The most frequently involved organs are the lungs.
An abnormal chest x-ray may or may not be accompanied by such overt symptoms as shortness of breath (especially upon exertion),
heaviness/tightness in the chest, and a dry, non-productive cough. These often result in a reduced exercise capacity. When the
nervous system is involved there may be a myriad of symptoms possible (see discussion below). Heart involvement is
often silent and may only be detected after death. Ocular involvement is quite frequent, so anyone suspected of having
sarcoidosis should have a complete eye examination at least once a year in order to prevent any unnecessary loss of sight. Eye
involvement may not be heralded by any overt symptoms at onset, but may also be indicated by somewhat dry, scratchy eyes. The most
common eye condition is uveitis. Skin conditions may vary as to type of lesion, body location, and severity/longevity
of the symptoms.
|
|
Initial sarcoidosis symptoms frequently appear in the lungs, and about 90% of all individuals who are diagnosed with
sarcoidosis will eventually have lung involvement. About half of the patients with more acute presentations will have a combination
of symptoms that together are called Lofgren's Syndrome. Lofgren's
Syndrome consists of three major elements, i.e. erythema nodosum, bilateral hilar (lymph)adenopathy, and polyarthralgias.
Erythema nodosum consists of tender/painful red raised nodules that
most often appear on the front of the leg between the knee and ankle (shins), predominantly in women in the springtime.
Bilateral hilar (lymph)adenopathy is characterized by inflammation/enlargement of the lymph nodes in the lungs near their inner border that
is easily and most commonly identified by a chest x-ray. Bilateral means that it's on both sides. Hilar comes from "hilum" which is the
area through which ducts, nerves, or blood vessels enter and leave a gland or organ (in this case, a lung). Adenopathy (often synonomous
with lymphadenopathy) refers to a glandular disease or enlargement of glandular tissue (especially a chronic, abnormal enlargement of the
lymph nodes/glands, usually associated with disease). Radiographics
presents a somewhat complicated but thorough discussion of certain aspects of pulmonary sarcoidosis that includes bilateral hilar
lymphadenopathy.
The third major element of Lofgren's Syndrome is the presence of
polyarthralgias, which are multiple joint aches sometimes referred to as arthritis, but not usually resulting in the destructive
joint changes present in true arthritis. They are more prominent in men. The "arthritis" is often acute, involves the lower extremities,
and may include such symptoms as extreme fatigue, general weakness, and low-grade fever.
The predicted outcome of Lofgren's Syndrome is generally favorable with about 90% of patients becoming disease-free within two years
and experiencing no further problems. In contrast, patients with other forms of sarcoidosis such as lupus pernio, a disfiguring skin
condition, cardiac sarcoidosis, or neurosarcoidosis rarely experience such disease remission.
|

|
Pulmonary (respiratory) sarcoidosis is classified in five stages (categories) based on chest x-ray findings (CXR).
It is important to emphasize that the term, stages, can be misleading in that patients do not always graduate from a mild case to a
more serious case. Stage one does not necessarily progress to stage two, three etc. This is why some physicians refer to these categories
as types or groups rather than stages, since they do not imply a progression; rather they are patterns seen on the x-rays. These
categories have been useful for prognosis (likelihood of improvement), but have a low correlation with symptoms and pulmonary function.
In many cases the disease remits and never returns.
A lengthy and in-depth article, "Sarcoidosis, A Primary Care Review"
includes a table that provides information about the differences in chest radiographs, pulmonary function tests, signs/symptoms, and
expectation of remission for the various stages of pulmonary sarcoidosis. The article appears in the December 1998 issue of
The American Family Physician magazine.
|
|
Despite the fact that about 90% of sarcoidosis diagnoses involve the lungs (pulmonary sarcoidosis), cardiac sarcoidosis
and neurosarcoidosis tend to be more serious. Both types are more likely to be chronic or recurring with a greater likelihood
they will end in death, but initial diagnosis is so difficult that many cases are not discovered until post-mortem. In both
cases Prednisone is usually considered to be the cornerstone of therapy, while immunosuppressant agents like methotrexate and
azathioprine can be used along with the corticosteroids or in their stead, if the corticosteroids prove to be ineffective or
present too many side effects.
"Neurosarcoidosis is a complication of sarcoidosis
in which inflammation occurs in the brain, spinal cord, and other areas of the nervous system.� About 10% of sarcoid
patients will have such neurologic involvement. Neurosarcoidosis can affect any part or the nervous system, i.e. the
central nervous system (CNS) that is comprised of the brain and spinal cord, as well as the peripheral nervous system
that is comprised of all the nerves that send messages between the CNS and all the organs in the body. Sudden, facial
weakness (facial palsy) is the most common neurological symptom and involves the nerves to the muscles of the face. Since
any part of the nervous system may become affected by neurosarcoidosis, the symptoms can be quite varied both in kind and
in number, which then requires that a wide variety of tests be considered to confirm a diagnosis. Neurologic involvement
may involve a single nerve, multiple nerves, or a general area, and the onset of symptoms may be sudden or gradual.
"Sarcoidosis involves almost every part of the body including the heart.
Cardiac sarcoidosis
is estimated to be present in 10-25 percent of patients with sarcoidosis." It can damage virtually any part of the heart
and may strike down an apparently healthy person with no prior warning, leaving it to the local coroner to determine
that the person�s demise was caused by cardiac sarcoidosis. Various types of CS include heart rhythm disorders, heart
failure, coronary disease, and pericardial disease (pericarditis). Various drugs used to treat cardiac sarcoidosis include
corticosteroids (Prednisone), immunosuppressants (methotrexate or azathioprine), and anti-malarials (Hydroxychloroquine
and chloroquine).
|

|
There is no single medical test or procedure that will absolutely diagnose the presence of sarcoidosis in a person. Normally,
various tests and procedures are conducted, both to rule out other disease conditions and to confirm the presence of sarcoidosis in the
patient. In addition, a complete medical history taking and thorough physical examination are a vital part of the diagnosis process.
Some of the best known tests and procedures that may be performed include: a chest x-ray, CT scan, pulmonary function tests,
bronchoscopy/transbronchial biopsy, and a gallium scan, all of which involve the lungs. Other tests that should/could be performed
include: ophthalmic evaluation with slit lamp exam (eyes), electrocardiogram and thallium scan (heart), tuberculin and Kveim-Siltzbach
tests (skin), and a biochemical panel (urine and blood) to evaluate kidney/liver functions and measure calcium levels.
Check out the Foundation for Sarcoidosis Research
site for more information about these tests.
|
|
Corticosteroids are the most common medications used to treat Sarcoidosis. They appear to be the most effective in relieving
many of the symptoms of the disease. The most common corticosteroid is Prednisone, which can cause significant side effects and
should only be used under the strict advice and supervision of your physician. Sometimes oral Prednisone is prescribed to be taken on
alternating days so that the side effects are minimized. Inhaled corticosteroids, which are generally prescribed for chronic lung
problems, are sometimes recommended over oral corticosteroids because they remain locally in the airway and thus cause fewer and lesser
side effects (rinse and gargle with water after each use to prevent thrush; usage may also cause hoarseness and/or sore throat). The
drawback is that there is little evidence that use of these inhaled corticosteroids results in any long-term improvement of sarcoid
symptoms. Two of these inhaled corticosteroids include budesonide, which is known as Pulmicort in Australia and Rhinocort
in the United States, and fluticasone propionate, which is known as Flixotide in Australia and Flovent or
Flonase in the
United States. Names of other corticosteroids include: triamcinolone, prednisolone, dexamethasone, beclomethasone, and deflazacort.
According to an article that was published in the March 1997 issue of the Chest Journal,
"Outcome in Sarcoidosis : The Relationship of
Relapse to Corticosteroid Therapy", authors Gottlieb, Israel, Steiner, Triolo, and Patrick stated that "74% of patients who
were adequately treated with systemic corticosteroids for severe symptoms of sarcoidosis appeared to be at lifetime risk for recurrence
of disease. Because of the risk of relapse, we recommend at least semiannual visits for those patients who are or who have been
treated with systemic corticosteroids. If corticosteroids predispose to clinical relapse, the implication would be to withhold treatment
from patients with newly diagnosed sarcoidosis unless symptoms and disability were compelling, and a similarly conservative approach
would be appropriate during relapse."
Important Note: The Arthritis
Foundation (among others) advises that people who take corticosteroids should NEVER decrease or stop them abruptly. Ceasing use of
the drug must occur slowly with close supervision by a doctor. The reason is that the body does not produce its own cortisone when
corticosteroid medications are present. If the drug was stopped abruptly, there would be no cortisone present in the body. This could
be fatal. When corticosteroids are stopped gradually, over a period of weeks to months, it gives the body time to adjust and start
producing cortisone on its own again. Patients taking corticosteroids should carry a card or preferably wear a bracelet indicating that
they are taking a corticosteroid.
Even though corticosteroids are the drugs of first choice in treating sarcoidosis, sometimes other drugs may need to be used with
or in place of them. The corticosteroids are generally considered to be the most effective treatment, but they can have rather
severe side effects or they may not be strong enough to suppress all the sarcoid symptoms by themselves. Therefore, there are other
drugs that can be utilized either individually or in combination. The best known corticosteroids such as Prednisone and Prednisolone.
Drugs in other classifications that have been used with mixed success include immunosuppressives such
methotrexate,
azathioprine,
cyclophosphamide, and
cyclosporine and antimalarials such as
hydroxychloroquine,
chloroquine, and
colchicine. For the most part they may provide
relief from some of the symptoms of sarcoidosis, but do not appear to have the overall beneficial effects of corticosteroids.
For tables listing many of the drugs used against sarcoidosis, what they are used for, and how to use them, check out the
Arthritis Foundation Website.
It provides great information that is grouped into a half-dozen categories. One of the categories is DMARDs, a term I am beginning
to see more often these days.
For those like me who were not familiar with this designation, DMARD (disease-modifying antirheumatic drug) is a drug which can
be used in the treatment of rheumatoid arthritis (RA). A number of drugs are considered DMARDs, and they can be used in a variety of ways,
depending on the specifics of a patient's situation and a doctor's usual approach to the treatment of RA. These drugs cannot cure
rheumatoid arthritis, but they can keep a patient more comfortable, and prolong the time in which a patient enjoys full functionality.
They can help the patient avoid complications of RA that tend to appear without DMARD treatment.
In addition to being used in the treatment of RA, DMARDs can also be employed in the treatment of a number of autoimmune conditions.
These drugs often have a suppressive effect on the immune system which is designed to prevent inflammation of the joints, thereby
reducing joint damage. The prevention of inflammation preserves joint function and keeps joints healthier, thus reducing pain and
stiffness for the patient. Therefore, both DMARDs and immunosuppressants are drugs that help to reduce inflammation and slow disease
progression.
|

|
Uveitis, is one of the more common conditions related to
having sarcoidosis and occurs in about 25% of those who have the disease. Very simply said, Uveitis is swelling and irritation of the
uvea, the middle layer of the eye. The uvea provides most of the blood supply to the retina. Beyond that uveitis presents in several forms,
some of which are closely connected to autoimmune diseases such as sarcoidosis. Because it is so common in those who have been diagnosed
with sarcoidosis, anyone suspected of having sarcoid should undergo a complete eye exam to rule out or confirm its presence.
According to the doctors at the Ocular Immunology
and Uveitis Service at the Massachusetts Eye & Ear uveitis is the third leading cause of blindness in the United States. They
further state that Uveitis is not a single disease. Inflammation in the eye may result from many different infectious agents. Or it may be
a manifestation of various systemic disorders, including sarcoidosis, some arthritic syndromes and chronic intestinal diseases. It can also
result from trauma to the eye. Uveitis is the most common eye problem encountered in people who have sarcoidosis. Uveitis based on
autoimmunity is the most common form and tends to be recurrent.
EyeSmart provides information from the American Academy
of Ophthalmology. The Web site contains substantial information about uveitis and contains a very nice diagram of the eye and its
parts. The Casey Eye Institute, Department of Ophthalmology is located on the campus of the
Oregon Health and Science University
and contains the Uveitis Clinic. The Casey Eye Institute is one of the world's leading uveitis research centers and explains
uveitis as follows. "Inflammation can occur anywhere in the body. In general, inflammation is the body's response to an injury.
Inflammation always involves the recruitment of white blood cells from circulation to the site of injury. White blood cells normally
circulate in the body and are vigilantly looking for an injury such as an infection or a wound. Although, uveitis can result from an
infection, for most patients, uveitis is thought to be occurring because white blood cells are responding to a signal that injury is
occurring even though no detectable infection is present. Since white blood cells are the major component of one's immune system,
often times uveitis is appropriately described as an autoimmune disease, a disease in which the body's own immune system attacks or
betrays itself."
An article about Uveitis at the
HealthAnswers Web site explained that the uvea is the middle layer of the eye, is very vascular and supplies blood to the retina.
The most common form of uveitis is anterior uveitis which affects the iris at the front of the eye. This condition is also
referred to as iritis or nongranulomatous uveitis. The disorder is associated with some autoimmune diseases, may affect only one eye,
and is most common in young or middle-aged people.
Posterior uveitis affects the back of the uveal tract and may involve the choroid cell layer or retinal cell layer or both.
This condition is also known as granulomatous uveitis, choroiditis, choroidoretinitis, or sometimes just retinitis. The inflammation
causes spotty areas of scarring that correspond to areas with vision loss. The degree of vision loss depends upon the amount and
location of the scarring. It can involve one or both eyes and is the form of uveitis most often associated with sarcoidosis and a
number of other specific diseases. Posterior uveitis is likely to last for months or even years and may cause permanent vision
damage even with early treatment.
Important Note: If a person is even suspected of having sarcoidosis, he/she should have a complete eye examination including
a slit lamp exam. If sarcoidosis is
confirmed, the individual should have a minimum of yearly eye exams and should have an exam at any other time that there is unusual
dryness, scratchiness, or other symptoms that are out of the ordinary. Uveitis can often be quite advanced by the time obvious symptoms
appear. Therefore, it is very important for individuals to act promptly if they have sarcoid and notice any unusual sensations in their
eyes.
|

|
IMPORTANT NOTE FOR ANYONE WITH ACTIVE SARCOIDOSIS! - If you answer "yes" to any of the following questions, read on. The information
provided here just may save your life.
- Do you believe that you do have or may have active sarcoidosis symptoms?
- Are you searching for a sarcoidosis specialist and/or sarcoidosis clinic?
- Do you have an urgent need to be seen by a sarcoidosis specialist?
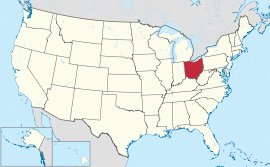
- Are you able to travel to Cleveland, Ohio (if you aren't sure where Ohio is
located in the U.S., the graphic of the U.S. shown here shows Ohio in red)?
|
Cleveland Clinic
Northern Ohio
|
Please understand that I am not advocating that anyone use the services of any particular sarcoid doctor or clinic, but when I visited
the Website for Cleveland Clinic, I was immediately excited. If you are just at the level of seeking information about sarcoidosis and
hospitals/clinics that specialize in the disease, visit
"Answering Your Questions About Sarcoidosis" where you can download an informational guide about sarcoidosis and view several
in-depth videos that will provide further information. If you then wish to schedule an appointment at the Cleveland Clinic, there is a
box at the bottom of the page that lists a toll free number and states that "to minimize multiple trips to Cleveland Clinic for diagnosis,
our schedulers arrange appointments with various specialists and tests within a few days."
If you decide that you have an urgent need to see one of the specialists at Cleaveland Clinic right away, visit their Web page,
"Same-Day Appointments"
where you will find this proviso: "Cleveland Clinic now offers same-day appointments. In most cases, depending on the level of care
you need and the time of day when you call [before noon], you'll be seen by a physician that day." The page provides extensive information
about the services they provide and locations where the services are offered.
For a myriad of other information about sarcoidosis and the Cleveland Clinic, be sure to run your mouse along the dark gray bar at the
top of most pages on the Website. Numerous listings of links to other pages will drop down and be just a click away. There are a number of
other good sarcoidosis clinics in this country now, but some of them have really "user UNfriendly" Websites where a user can go "round
and round" the Website without ever finding the information they are seeking. If the Cleveland Clinic and its staff are anywhere near
as good as their Website, those of us with sarcoidosis have found a real winner.
|

Back to top // Sarcoid Connection Home

Questions and comments about this Web site and/or sarcoidosis are always welcome.
You may either send me an E-mail message or leave an entry in Visitor Comments.

cmtown@excite.com
|
![]()
![]()
![]()